Acrocyanosis
Last edited on : 19/11/2023
Acrocyanosis is a permanent vascular acrosyndrome characterized by a painless cyanotic (usually bluish) discoloration of the extremities, which may be accentuated by cold or emotion. It may be primary (idiopathic) or, more rarely, secondary to another pathology.
Etiologies
Primary acrocyanosis
Primary acrocyanosis is the most common acrosyndroma, and is always benign. It most frequently affects women, adolescents and adults under the age of 30. It tends to resolve spontaneously around the age of 40-50. Its cause is unknown, but a genetic determinism is presumed.
Secondary acrocyanosis
Secondary acrocyanoses are thought to be rare, and should be considered in the face of atypical clinical presentations or particular contexts. There are many possible etiologies:
- Hypoxemia: cyanogenic heart disease, pneumopathy, smoking
- Connectivites and vasculitides: granulomatosis with polyangiitis, systemic lupus erythematosus, rheumatoid arthritis, Buerger's, etc.
- Neoplasia and hematological disorders
- Occlusive arteriopathies
- Drugs and toxic substances
- Spinal cord lesions
- Genetic or chromosomal malformations and metabolic disorders
- Vascular dysautonomic syndromes (e.g. postural orthostatic tachycardia syndrome)
- Psychiatric and eating disorders (anorexia)
Diagnosis and clinic
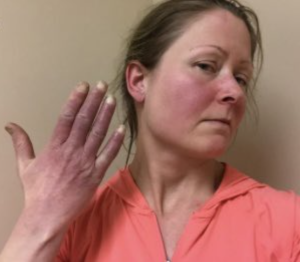
Acrocyanosis (hands and face) in a patient with postural orthostatic tachycardia syndrome
- Positive diagnosis is exclusively clinical. In its typical form, primary acrocyanosis is manifested by :
- Uniform bilateral cyanosis (blue to red), permanent but varying in intensity. It most frequently involves the fingers up to the wrists, but may be associated with involvement of the feet up to the legs, nose, face or ears.
- Increases with cold and emotions. Improves with heat and/or elevation of the limb. Painless at room temperature.
- Coldness on examination, sometimes discrete oedema +- hyperhidrosis (sometimes very severe, requiring consultation). Discoloration on pressure, progressive recoloration.
- Arterial and trophic examination is always normal.
Raynaud's phenomenon may be associated.
Any other abnormality (particularly unilateral presentation, head-only, generalized, clinical pain, trophic or arterial abnormalities) should prompt consideration of secondary acrocyanosis or another diagnosis.
Clarification and differential diagnosis
No further investigations should be carried out in the case of typical clinical findings in adolescents or young adults. Otherwise, review the diagnosis and consider: capillaroscopy +- examinations according to clinical orientation.
Differential diagnoses are easily evoked on a clinical basis. Main signs to look for :
- Trophic disorders / signs of vasculitis → scleroderma? Lupus ? Cryoglobulinemia ?
- Generalized cyanosis → cyanogenic heart disease ? Chronic respiratory insufficiency ? Polyglobulia ?
- Acrocyanosis limited to one limb → angiodysplasias ? Complex regional pain syndrome (++ pain-dominant clinic) ?
- Association with hard, cold, painless, limited edema → self-aggression (++ garots) in a psychiatric context?
If associated with Raynaud's phenomenon, investigate appropriately.
Therapeutic management - Treatments
- Reassurance (benign phenomenon) in case of primary acrocyanosis
- Symptomatic management:
- Avoidance of and protection from cold, cessation of smoking, physical exercise.
- Psychological care if necessary. Psychiatric treatment in the case of anorexia nervosa.
- Treatments for hyperhidrosis should be reserved for cases that represent a real socio-professional handicap.
- First-line treatment: ionization sessions (physical medicine).
- Second-line treatment: endoscopic sympathectomy
- Management of associated Raynaud's disease (see specific chapter) or etiology in the case of secondary acrocyanosis.
Author(s)
Dr Shanan Khairi, MD
Bibliography
EMC, Traité d'Angéiologie, Elsevier, 2014
Creager M et al., Vascular Medicine: A Companion to Braunwald’s Heart Disease, Saunders, 2013